흡수성 판의 잔여물: 지속적인 비첨 감염 및 변형의 드문 원인
An Infected Absorbable Plate: A Rare Source of Persistent Tip Infection and Deformity
Article information
Trans Abstract
Neglecting timely and appropriate management of foreign body-related infections can lead to significant changes in the skin and soft tissue. We present here a case of a 28-year-old female with persistent discharge from a defective nasal tip and a columellar wound. She had previously undergone silicone dorsal augmentation and tip plasty with ear cartilage, followed by implant removal and wound irrigation due to infection. Despite silicone removal, the infection persisted, resulting in severe tip and columellar defects. We managed the infection by removing substantial absorbable plate debris and suture material from the caudal septum and tip. Subsequent framework reconstruction using rib cartilage and a forehead flap successfully restored the normal shape of the nose. This case highlights that an absorbable plate can act as a foreign body harboring infection, warranting thorough exploration and removal of remaining debris.
Introduction
Recently, various types of absorbable plates, often in the form of battens or septal extension grafts, have been utilized in rhinoplasty. Although surgeons are aware that alloplastic materials like silicone or Gore-Tex implants can cause infections, necessitating immediate removal when conservative treatment fails [1,2], they may overlook absorbable plates, assuming they will naturally resorb. However, these plates are foreign bodies that can potentially cause infections until fully absorbed. Delayed treatment of an infection caused by an infected absorbable plate can lead to significant defects in the surrounding soft tissue [3].
Here, we report a case of nasal tip and columellar defects caused by an overlooked infected absorbable plate. The infection was successfully managed by foreign body removal, and the defect was reconstructed using a rib cartilage and forehead flap.
Case
A 28-year-old female patient was referred due to uncontrolled infection and defects in the tip and columella. The patient had previously undergone four rhinoplasties at different clinics. Her clinical and surgical history is summarized in the timeline (Fig. 1). Six years earlier, she underwent rhinoplasty with a silicone dorsal implant and tip plasty using ear cartilage. Two years later, swelling of the dorsum occurred; however, the patient underwent revision rhinoplasty without implant removal. Subsequently, nostril asymmetry and a pinpoint tip defect developed, leading to a third rhinoplasty at another clinic to correct the nostril asymmetry. However, the reinserted silicone implant had to be removed owing to an immediate postoperative infection. Even after the silicone was removed, the tip swelling and pus discharge persisted, requiring repeated wound irrigation via an open approach. Despite the silicone removal and administration of empirical antibiotics, the infection continued, and skin contracture developed, resulting in a tip defect. Stem cells were injected into the wound two to three times a month over a year but there was no improvement. The patient then underwent a fourth rhinoplasty using ear cartilage to correct the contracted tip defect, but the infection worsened.
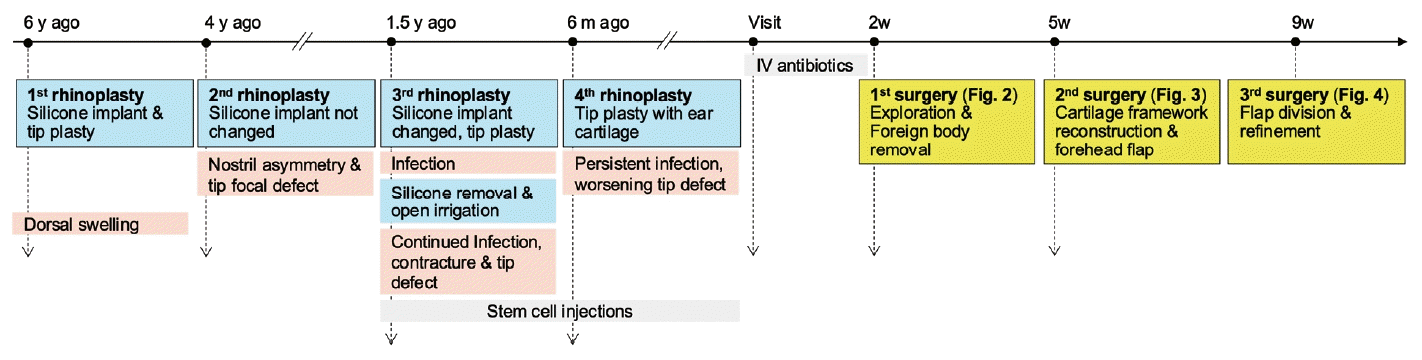
Timeline of clinical and surgical history. The timeline summarizes the patient’s clinical course, including four rhinoplasties performed at other clinics over 6 years and subsequent surgeries at our clinic consisting of foreign body removal, cartilage framework reconstruction and a forehead flap, and flap division. Blue boxes, surgeries performed at other clinics before visiting our clinic; yellow boxes, surgeries performed at our clinic; pink boxes, patient complaints; gray boxes, conservative treatments.
When the patient visited our clinic, she had a short, upturned nose with a defect at the tip, from which pus was drained upon compression (Fig. 2A). Bacterial culture of the discharge revealed Pseudomonas aeruginosa. Despite administering appropriate antibiotics for 1 week based on the sensitivity profile, the infection persisted. The wounds were then explored.
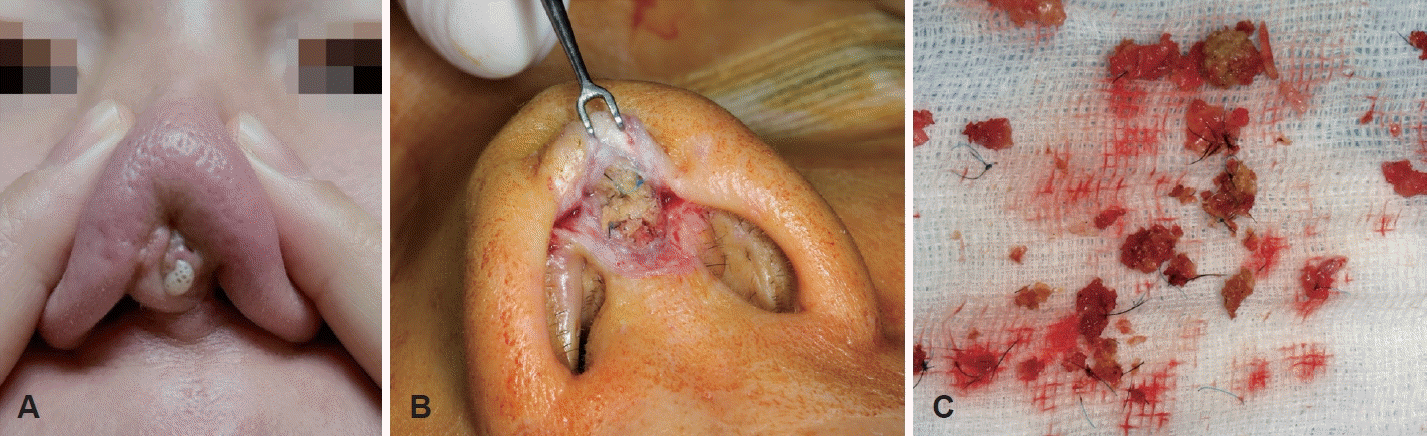
First surgery. Exploration of a 28-year-old female patient with persistent discharge from the nasal tip and columellar defect. A: Pus discharge observed upon squeezing the nasal tip. B: Intraoperative view revealing abundant absorbable plate debris and multiple polypropylene sutures within the defective nasal tip. C: Removed debris consisting of absorbable plate fragments and suture materials.
First surgery
Exploration of the tip revealed a significant amount of infected absorbable plate debris and numerous polypropylene suture materials beneath the defect, from which pus was drained (Fig. 2B). The debris occupied the entire columella (approximately 6 mm wide), far exceeding the typical plate thickness. In the sagittal plane, it spanned most of the caudal septum, extending over 10 mm. All foreign materials were removed (Fig. 2C), and further exploration and thorough irrigation were performed.
Second surgery
Reconstruction was planned as a staged operation after the inflammation had completely subsided, approximately 3 weeks after foreign body removal. Scar tissue at the tip and columella was meticulously excised, with careful attention paid to the aesthetic subunit (Fig. 3A and B). The tip support structures, including the entire medial and intermediate crus, part of the lateral crus of the lower lateral cartilage, and a substantial part of the caudal septum, were destroyed due to the longstanding infection. To reconstruct the cartilaginous framework, the right sixth costal cartilage was harvested. Bilateral extended spreader grafts, septal extension grafts, bilateral alar contouring grafts, and an additional dorsal onlay graft were used to reconstruct the tip framework (Fig. 3C and D). A right paramedian forehead flap was used to cover the tip and columellar defects (Fig. 3E and F).
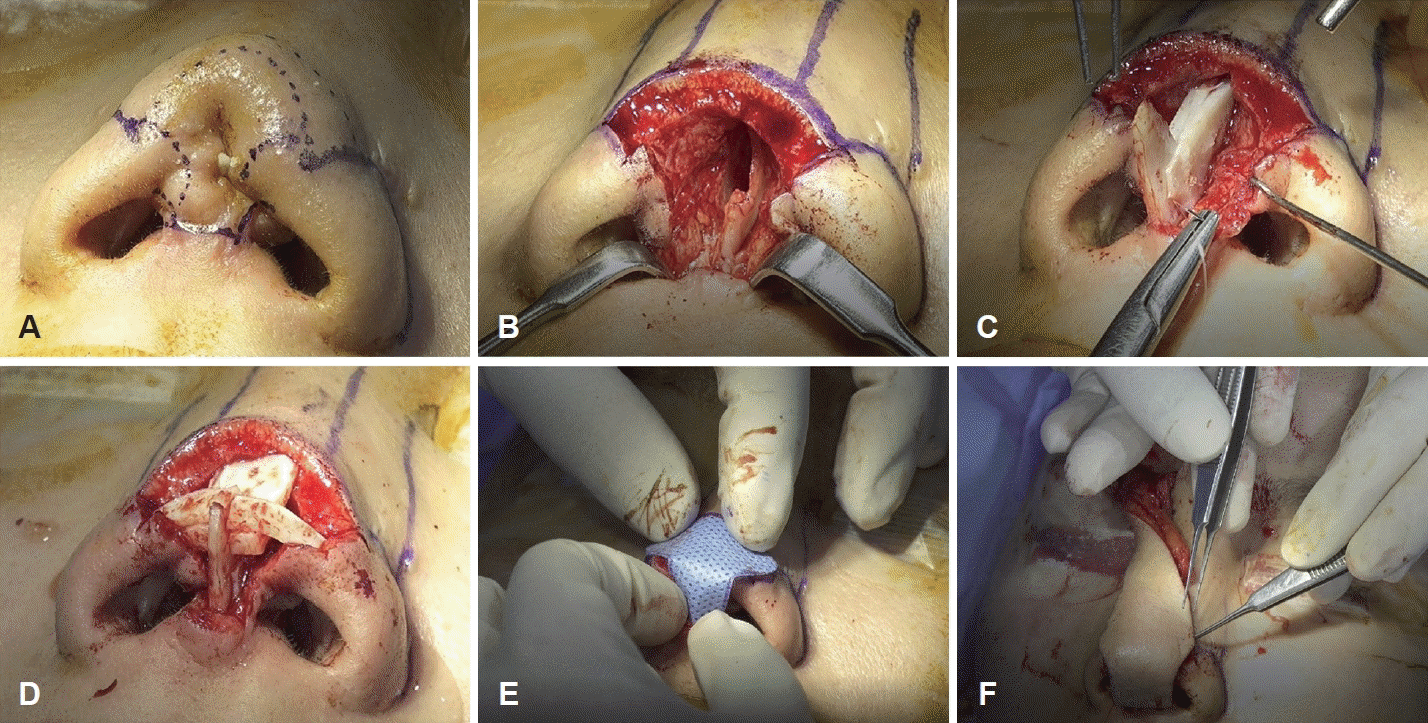
Second surgery. Reconstruction of the tip and columellar defect using costal cartilage and a forehead flap. A and B: Scar tissue excision following the aesthetic subunit. Extensive damage to the lower lateral cartilages and caudal septum observed. C and D: Cartilaginous framework reconstructed with various grafts. E and F: Defect coverage achieved with a right paramedian forehead flap.
Third surgery
Four weeks following surgery, adequate blood supply and successful flap engraftment were confirmed, after which flap division was performed. The forehead area was sutured with tension to prevent drooping of the eyebrows (Fig. 4A). The flap thickness was adjusted through appropriate defatting to match the margins (Fig. 4B and C).
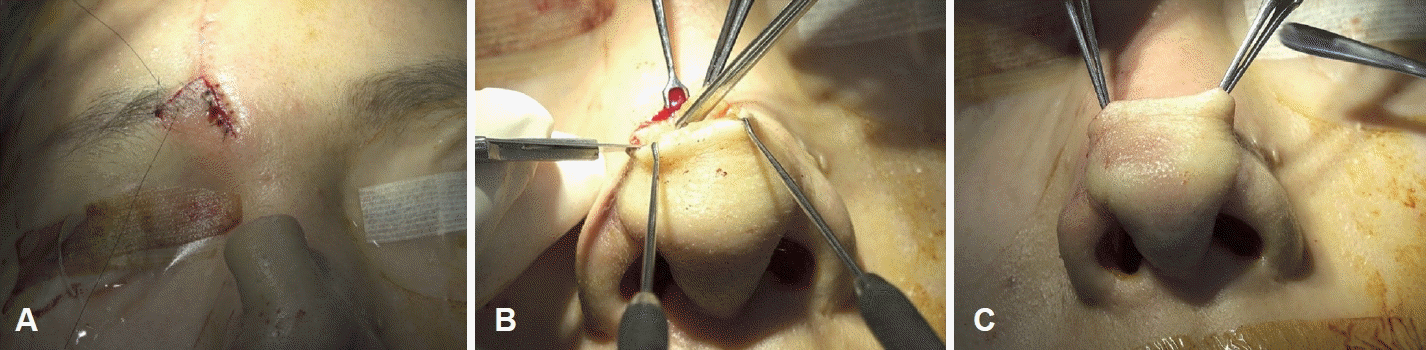
Third surgery. Forehead flap division and refinement of the nasal side flap. A: Suturing of the forehead area was performed under tension to prevent eyebrow drooping. B and C: Flap thickness adjusted via defatting for contour matching.
After surgery, the defects in the tip and columella were successfully reconstructed, and the previously contracted nose shape improved (Fig. 5). The forehead scar where the flap was harvested was deemed acceptable, and the patient expressed utmost satisfaction with the surgical outcomes.
Discussion
Surgeons from the previous surgeries presumed that removing the foreign body (silicone implant) would resolve the infection. However, they overlooked that the absorbable plate used on the caudal septum for tip modification could be a potential source of infection. Thus, further exploration of the caudal septum was not conducted. When the patient visited our clinic, immediate surgical exploration without attempting intravenous antibiotics could have been an option given that persistent infections always have underlying causes. However, the authors believe that trying intravenous antibiotics based on sensitivity test was a reasonable choice.
Absorbable plates made of biodegradable polymers, such as polydioxanone or polycaprolactone, are commonly used for structural support in septoplasty and rhinoplasty [4,5]. These plates degrade through hydrolysis, but their complete resorption can take up to 25 months [6]. Due to this prolonged degradation period, they pose risks of infection and inflammation until fully resorbed [3]. Recently developed, three-dimensional-printed absorbable plates have scaffold structures that support tissue ingrowth and regeneration. These relatively thick plates are slow to resorb, making them susceptible to infection.
There are many reports on the successful use of absorbable plates in septorhinoplasty [4,5,7], but reports of complications are rare [3]. Many surgeons may believe that the absorbable plates can be safely used and cause no complications because of the scarcity of complication reports. However, the authors believe that this does not necessarily indicate that all absorbable plates can be used as safely as autologous material.
In general, thin and small absorbable plates used in places with optimal soft tissue envelope and good blood supply resorb with time and are less likely to develop complications [4,5,7]. However, large and thick plates used as an extension graft with tension, or in areas with relatively poor circulation such as the tip and columella of multiply revised nose, resorb very slowly and have high chances of complications such as infection or surrounding tissue necrosis.
In this patient, the neglected presence of infected plates in previous revision surgeries caused cartilage necrosis and significant soft tissue defects. With perception of possible complications of absorbable plates, judicious exploration and optimal removal of these infected plates could have prevented such a disastrous event.
As for the suture materials used, while absorbable polydioxanone sutures are more prone to inflammation than nonabsorbable polypropylene sutures owing to their hydrophilic nature [8], a meta-analysis demonstrated no difference in the development of infection [9]. We believe that the source of infection was the absorbable plate rather than the suture material used in this case. However, similar to other foreign bodies, excessive use of suture materials can increase the risk of infection; thus, it is advisable to use them minimally.
The timing of the revision rhinoplasty after implant removal depends on several factors. Commonly, revision rhinoplasty is performed as a staged operation after complete infection control [1]. Immediate reconstruction with autologous tissue at the time of alloplast removal has also yielded excellent cosmetic results [1]. However, in cases where pus discharge is persistent and the skin is severely damaged, delaying the surgery until all infections are fully controlled and active inflammation subsides is recommended [10]. In this patient, the authors opted for a safe approach, given that the active inflammation accompanied by pus discharge persisted for more than a year.
The choice of reconstruction method for tip and columellar defects depends on the defect size, depth, and location. Small defects may be addressed with a local flap [11], while larger ones exceeding 2 cm or involving multiple subunits may require a forehead flap [12,13].
In this case, the defects extended beyond 2 cm after framework reconstruction and encompassed multiple subunits including the tip, columella, and bilateral soft tissue facets, necessitating a forehead flap [12]. Although a melolabial flap can be an alternative option, it is not large enough to cover the defect considering the defect size, location, and depth. In addition, the scar around the mouth corner developing after melolabial flap is aesthetically poorer than the forehead flap scar in this relatively young patient.
While reconstruction does not always need to follow the subunit principle [13], this approach is particularly beneficial for convex surfaces such as the tip and columella, as demonstrated in this case [14]. Indeed, the subunit-based reconstruction using a forehead flap provided adequate coverage without distorting the contour, yielding an excellent aesthetic outcome.
This case demonstrates that an absorbable plate in the nose can serve as a neglected source of infection. The suspicion of foreign bodies and early exploration are required to remove the plates when an infection persists, even with proper management. Large tip and columellar defects were successfully reconstructed using a forehead flap and rib cartilage.
Notes
Acknowledgments
None
Author contributions
Conceptualization: Hong Ryul Jin. Data curation: Hong Ryul Jin, Su Jin Kim. Investigation: Hong Ryul Jin, Su Jin Kim. Visualization: Hong Ryul Jin, Su Jin Kim. Writing—original draft: Hong Ryul Jin, Su Jin Kim. Writing—review & editing: Hong Ryul Jin, Su Jin Kim.

