Perceptions and Concerns Regarding Over-the-Counter Hearing Aids Among the Public, At-Risk Individuals, and Audiology Professionals in Korea
Over-the-Counter (OTC) 보청기에 대한 일반인, 난청 위험군 및 청각 전문가의 집단간 인식 비교 연구
Article information
Abstract
Background and Objectives
Despite increased global attention to hearing loss and the proven benefits of hearing aids, the access to adopting the device remains suboptimal for people hard of hearing, particularly in Korea. Over-the-Counter (OTC) hearing aids, recently introduced in the United States, are expected to lower barriers to access. This study aimed to compare, prior to national implementation, perceptions, concerns, and expectations regarding OTC hearing aids among the general public, individuals at risk for hearing loss, and audiology professionals.
Subjects and Method
A cross-sectional survey was conducted with 200 participants divided into five groups: adults aged 20-50, adults over 60, people at risk for hearing loss, licensed audiologists, and audiology students. Each group completed a validated questionnaire addressing the knowledge, interest, safety, self-adjustment, service concerns, counseling, and efficacy of OTC hearing aids.
Results
Audiologists and older adults expressed significant concerns about the absence of professional involvement, potential misdiagnosis, difficulties in device handling, and diminished service quality. Meanwhile, younger adults and those at risk of hearing loss were more neutral or optimistic, but they nonetheless demonstrated limited awareness and interest. All groups recognized the potential for improved accessibility through OTC hearing aids; however, concerns about consumer protection, self-management, and lack of counseling were substantial, especially among professionals and older adults.
Conclusion
While OTC hearing aids may enhance accessibility in Korea, our findings indicate a strong need for targeted education, enhanced consumer protection, and multidisciplinary support systems to ensure safe and effective adoption. Policymakers should consider these group-specific attitudes in strategies for successful integration.
Introduction
Hearing loss is a major public health challenge whose importance is increasing worldwide with population aging. The World Health Organization has reported that approximately 430 million people require hearing rehabilitation due to hearing loss and that hearing loss ranks as the fifth leading cause among conditions contributing to the global burden of disability [1]. In particular, in Korea, which is entering a super-aged society, approximately 35% of the population aged 65 years and older experience age-related hearing loss, and the burden continues to increase mainly among older adults [2]. Because hearing loss is directly linked not only to reduced hearing but also to secondary health problems such as social isolation, depression, cognitive decline, and decreased quality of life, early intervention and management have become urgent public health priorities.
Hearing aids are a representative rehabilitation tool for managing hearing loss, and their clinical effectiveness has already been sufficiently demonstrated. However, the actual uptake and usage rates remain very low. In Korea, the hearing aid purchase rate is 17.4% and the actual usage rate is only 12.6%, which creates a serious gap in hearing rehabilitation for individuals with hearing loss [3]. In the United States, only about 25% of adults with hearing loss wear hearing aids [4]. The low uptake has been attributed to multiple factors acting in combination, including high costs of hearing aids, social stigma, and lack of awareness of their necessity [5].
As one solution to address these limitations, the US Food and Drug Administration introduced the Over-the-Counter (OTC) hearing aid system in 2022, which allows direct purchase without a prescription through diverse distribution channels such as pharmacies and online and offline markets [6]. OTC hearing aids are available without a prescription for adults with mild to moderate hearing loss and are characterized by allowing consumers to use and adjust programming on their own [7]. The introduction of this system may lead to meaningful changes by expanding healthcare access, reducing economic burden, and increasing consumer choice. At the same time, because healthcare professionals are not involved, OTC hearing aids may also lead to new problems, such as worsening hearing loss, missed diagnosis of otologic diseases, and lack of appropriate counseling and fitting.
In practice, expert opinions on the introduction of OTC hearing aids are mixed. In a study by Midey, et al. [8] targeting pharmacists, insufficient education on hearing aid information and inadequate preparation for counseling were identified as concerns. In a study by Manchaiah, et al. [6] systematic education and provision of information were emphasized as necessary for counseling by hearing professionals and consumer protection. In contrast, from the consumer perspective, expectations are high with respect to affordability and improved accessibility [9]. In particular, the potential to reduce barriers to hearing aid use in regions where professional services are difficult to access or among groups with high cost burdens has been highlighted as a positive effect [10]. As such, prior studies abroad have reported that perceptions, concerns, and actual usage experiences vary widely among both consumers and professional groups when OTC hearing aids are introduced. In Korea, however, the OTC hearing aid system has not yet been officially implemented, and there is no study that comprehensively investigated perceptions across groups prior to implementation. There is a lack of empirical research comparing various stakeholders such as the general public, high-risk groups for hearing loss, and audiology professionals.
Accordingly, this study aimed to compare and analyze psychological and practical factors—such as perceptions, concerns, and expectations—regarding the introduction of OTC hearing aids among multiple groups, including the general public, individuals at risk for hearing loss, licensed audiologists, and audiology students. Through this work, we expect to provide policy and educational foundational data for future national introduction and market establishment of OTC hearing aids and to provide evidence for group-specific differentiated support strategies and consumer protection systems based on differences by age, risk group status, and professional background.
Subjects and Methods
Study participants
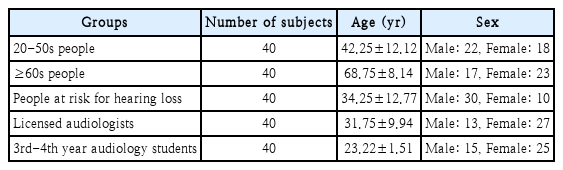
This study was conducted with 200 participants across five groups including the public aged 20 to 50 years, the public aged 60 years and older, individuals at risk of hearing loss, licensed audiologists, and audiology students. Forty participants were recruited for each group. The at-risk group included individuals discharged from military service, long-term workers exposed to occupational noise, and music-related practitioners, and all participants in this group had been exposed to noise for at least the past 5 years were selected (Table 1).
Participants were recruited through online announcements, and a non-probability convenience sampling method was applied to individuals who responded voluntarily. All participants submitted written informed consent after receiving sufficient explanation of the study purpose and procedures. The study procedures were conducted with approval from the Hallym University Institutional Review Board (IRB No. HIRB-2024-074).
Survey instrument
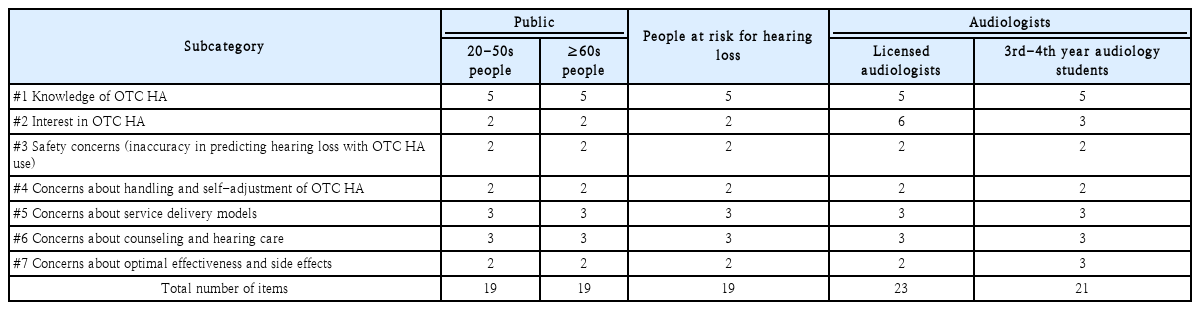
The questionnaire was translated and back-translated based on the National Survey of Pharmacist Awareness, Interest, and Readiness for Over-the-Counter Hearing Aids [8] and was then adapted to the domestic context where OTC hearing aids are not yet common. It included seven domains regarding OTC hearing aids, knowledge, interest, safety, concerns about handling and self-adjustment, service delivery model concerns, counseling, and efficacy, with a total of 18 to 24 items. Additional items were included for audiology professionals and the at-risk group to increase precision in assessing current status (Table 2). All items underwent expert review and a pilot survey to establish content validity and reliability (Cronbach’s α=0.83).
Study procedure
After explaining the definition and characteristics of OTC hearing aids to participants, understanding was confirmed and the survey was administered. This explanation by the researchers was provided to facilitate understanding in the Korean context where OTC hearing aids are not yet widespread, and biased content that could influence results was excluded as much as possible.
The 20 to 50 years groups (public, at-risk group, licensed audiologists, and students) responded online using Google Forms, whereas the older adult group aged 60 years and older responded offline using paper questionnaires. All surveys were administered face-to-face by the researchers to maintain consistency in survey mode and item content across groups. This approach was intended to improve response convenience, secure data quality, and facilitate analysis. The survey took approximately 5 minutes.
Data analysis
In the study design stage, items allowing duplicate responses were included to reflect diverse perceptions and experiences more broadly. All data were preprocessed using R software (version 4.4.1; R Foundation for Statistical Computing) and the dplyr package (version 1.1.4; Posit Software, PBC). Frequency and percentage analyses were then conducted by group and by item. Group differences for each item were explored by visualizing response distributions withcumulative bar graphs, and missing values and outliers were reviewed prior to analysis. To evaluate statistical significance of differences in response distributions across groups (n=40 per group), chi-square (χ2) tests of independence were performed for nominal and ordinal scale responses. P-values were calculated, and differences were considered statistically significant when the p-value was less than 0.05 (Supplementary Table 1, Supplementary Figs. 1 and 2).
Results
Knowledge of OTC hearing aids
Fig. 1 shows the percentage of “Yes” responses to subquestions on hearing aid knowledge across the five groups. In most groups, awareness was very high for “Do you know what a hearing aid is?” and “Do you know when and for whom a hearing aid is needed?” However, chi-square tests indicated statistically significant differences between groups for both items (p=0.024 and p<0.001, respectively), and the response rate for “When and for whom a hearing aid is needed” was somewhat lower in the public aged 60 years and older. In contrast, awareness was relatively low in younger adults and the at-risk group for “Do you know how to purchase a hearing aid and the process involved?,” “Are you aware that an adjustment period is necessary after purchasing a hearing aid?,” and “Do you know the difference between a conventional hearing aid and an OTC hearing aid?,” whereas licensed audiologists and students showed very high awareness. Statistical analyses showed highly significant differences between groups for all three items (p<0.001). These findings indicate meaningful differences in awareness of practical, hearing-aid-related information according to age and audiology expertise.
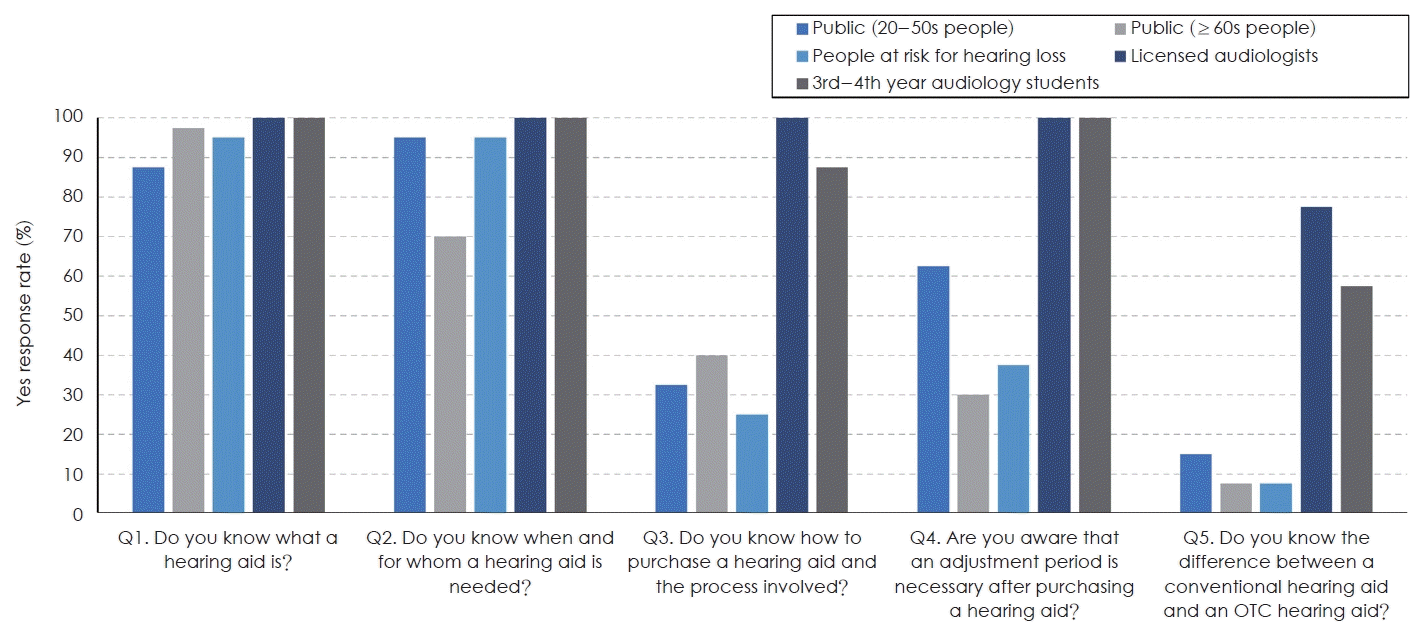
Level of knowledge about hearing aids by group. Proportion of “Yes” responses to questions about hearing aid knowledge among the five participant groups (younger adults, older adults, at-risk individuals, audiologists, students). Higher rates in audiologists/students, lower for lay groups. OTC, Over-the-Counter.
Interest in OTC hearing aids and information needs
Half of the public aged 20 to 50 years were interested in information about OTC hearing aids, whereas 62.5% of the public aged 60 years and older reported no interest. The at-risk group showed lack of interest in 82.5%. In contrast, licensed audiologists (57.5%) and students (77.5%) showed high interest in obtaining information. Thus, interest in information about OTC hearing aid differed clearly by group, and the distribution of interest levels differed significantly between groups (p<0.001).
For the item on interest in supporting individuals with hearing loss, students (77.5%) were highest, and approximately 72.5% of the public aged 60 years and older and the at-risk group also responded positively. In contrast, the public aged 20 to 50 years and licensed audiologists each showed 55.0% interest, but negative responses (10.0%) were relatively prominent in the public aged 20 to 50 years. In addition, 62.5% of licensed audiologists opposed financial support for OTC hearing aids, whereas 75.0% responded positively to the need for professional education in the workplace. Willingness to provide services was dispersed across responses (neutral 40.0%, negative 37.5%, positive 22.5%). The proportion reporting knowledge for counseling differed across groups, 62.5% in licensed audiologists and 25.0% in students, indicating a gap in practical readiness between groups. Response distributions for these items all showed statistically significant group differences (p<0.05), suggesting that attitudes toward OTC hearing aid information and support vary considerably by age and expertise.
Safety concerns and concerns about lack of professional involvement
For the question “Do you think OTC hearing aids are not effective in preventing hearing loss?,” licensed audiologists, students, and the public aged 60 years and older showed high proportions of “strongly agree” and “agree” responses, 67.5%, 57.5%, and 72.5%, respectively, indicating considerable skepticism regarding hearing loss prevention by OTC hearing aids (Fig. 2A). In contrast, the public aged 20 to 50 years and the at-risk group most frequently responded “neutral,” 62.5% and 42.5%, respectively, indicating no clear opinion or a more neutral perception. Notably, “disagree” and “strongly disagree” responses were a minority in all groups. A chi-square test confirmed that differences in response distributions across groups were statistically significant (p=0.0006), suggesting that evaluations of OTC hearing aid accuracy differed greatly by age and expertise.
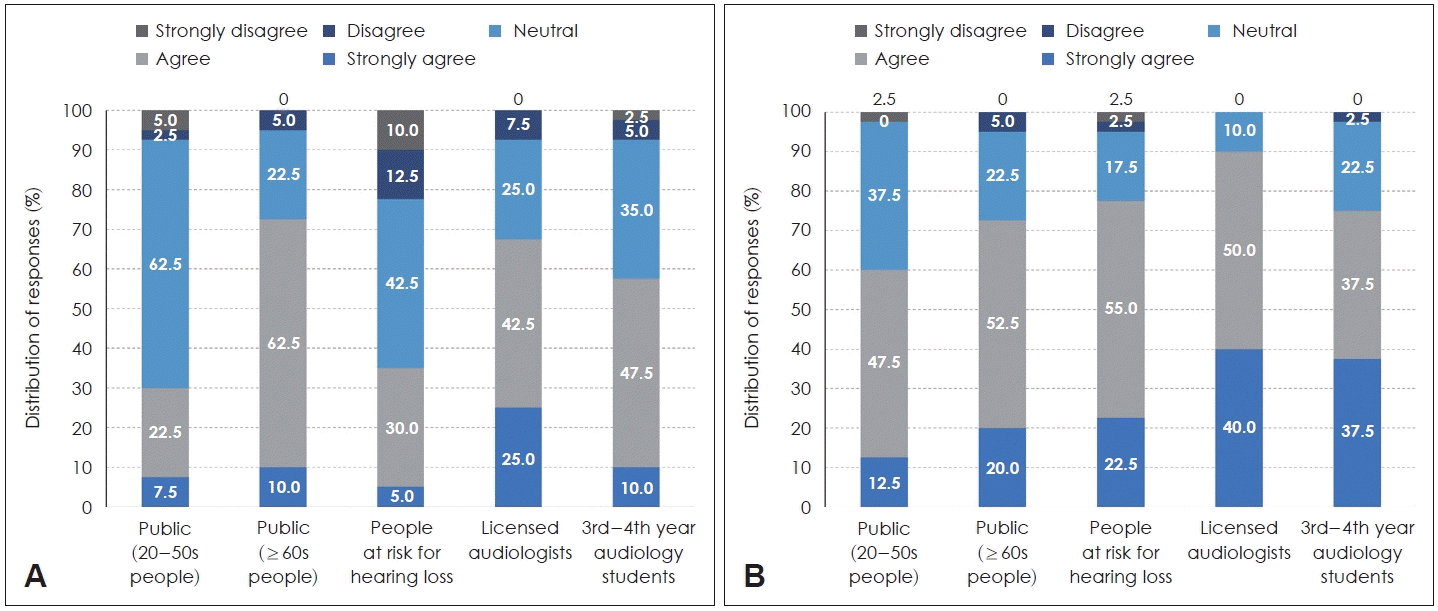
Participant perceptions of safety risks and absence of expert intervention. A: Perceptions of OTC hearing aids’ accuracy in predicting hearing-loss prevention. Percentage distribution of responses to the statement: “OTC hearing aids are inaccurate at predicting prevention of hearing loss.” Higher values indicate greater skepticism, especially among older adults and healthcare professionals. B: Concerns about missed diagnosis of ear diseases without expert examination. Proportion of each group agreeing that diseases other than hearing loss could be missed by use of OTC hearing aids without professional examination. OTC, Over-the-Counter.
For the item “Do you think OTC hearing aids without professional examination may miss detection of otologic disease other than hearing loss?,” the proportions of “strongly agree” and “agree” were very high across all groups (minimum 60.0%, maximum 90.0%), indicating strong recognition of the need for professional examination by healthcare providers prior to use (Fig. 2B). In particular, licensed audiologists (90.0%) and students (75.0%) emphasized its importance clearly, and the at-risk group and the public aged 60 years and older also showed agreement in more than 70%. “Neutral” responses were relatively higher in the public aged 20 to 50 years (37.5%), but overall, negative responses were very few. Although no clear significant difference between groups was observed for this item (p=0.094), all groups were analyzed as having a high consensus on the need for professional diagnosis.
Concerns about handling and self-adjustment of OTC hearing aids
Perceptions of difficulty in self-inserting OTC hearing aids differed clearly by group (Fig. 3A). In the public aged 20 to 50 years, about half (47.5%) showed a neutral attitude, and some (30.0%) anticipated difficulty, but strong concern (“strongly agree” 5.0%) was rare. Thus, younger adults generally perceived insertion burden as not large. In contrast, in the public aged 60 years and older, “agree” (35.0%) and “strongly agree” (22.5%) together exceeded half, indicating that older adults perceived greater difficulty in self-wearing. In the at-risk group, most (60.0%) responded “neutral,” showing dispersed perceptions. Licensed audiologists showed similar proportions of neutral (42.5%) and “difficult” (37.5%) responses, reflecting caution based on clinical experience. Students showed prominent “difficult” responses (50.0%), indicating higher evaluation of technical difficulty as pre-professionals. Chi-square testing confirmed statistically significant differences between groups (p=0.0038), suggesting practical perception gaps by age and expertise.
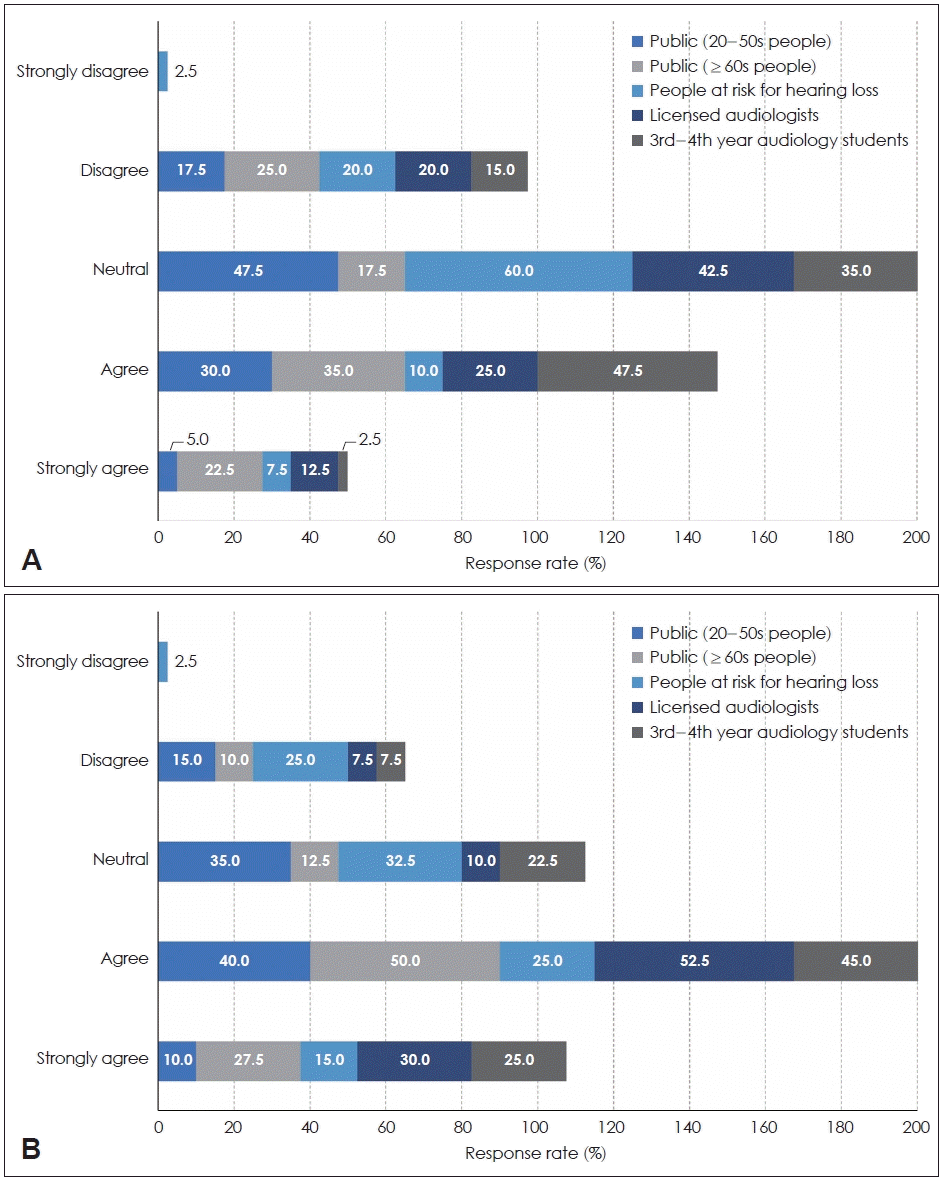
Concerns about handling and self-adjusting OTC hearing aids. A: Perceived difficulty of self-inserting OTC hearing aids. Participant perceptions of the ease or difficulty of self-inserting OTC hearing aids, by group. Greater perceived difficulty in older adults and professionals. B: Perceived difficulty of self-adjustment (volume/function) of OTC hearing aids. Respondent agreement with the difficulty of adjusting OTC hearing aids independently, highlighting increased concern in audiologists, students, and older adults. OTC, Over-the-Counter.
Clear group differences were also observed in perceived difficulty of self-adjustment of OTC hearing aids, such as volume and functions (Fig. 3B). In the public aged 20 to 50 years, “agree” (40.0%) and “neutral” (35.0%) were most common. In the public aged 60 years and older, “strongly agree” (27.5%) and “agree” (50.0%) totaled 77.5%, showing more prominent operational burden in older adults. In the at-risk group, about 40% expected difficulty in self-adjustment, with “strongly agree” (15.0%) and “agree” (25.0%). Licensed audiologists showed very high concern, with “strongly agree” (30.0%) and “agree” (52.5%) totaling 82.5%. Students also evaluated operational difficulty as high, with 70.0% in “strongly agree” (25.0%) and “agree” (45.0%). This result also showed a statistically significant group difference (p=0.019), indicating that perception differences by age, expertise, and hearing risk status exist in practice. Overall, concerns and perceived burden regarding handling and self-adjustment of OTC hearing aids differed significantly by age, hearing loss experience, and expertise, and higher levels of concern were consistently observed in older adults and professionals.
Service and counseling concerns
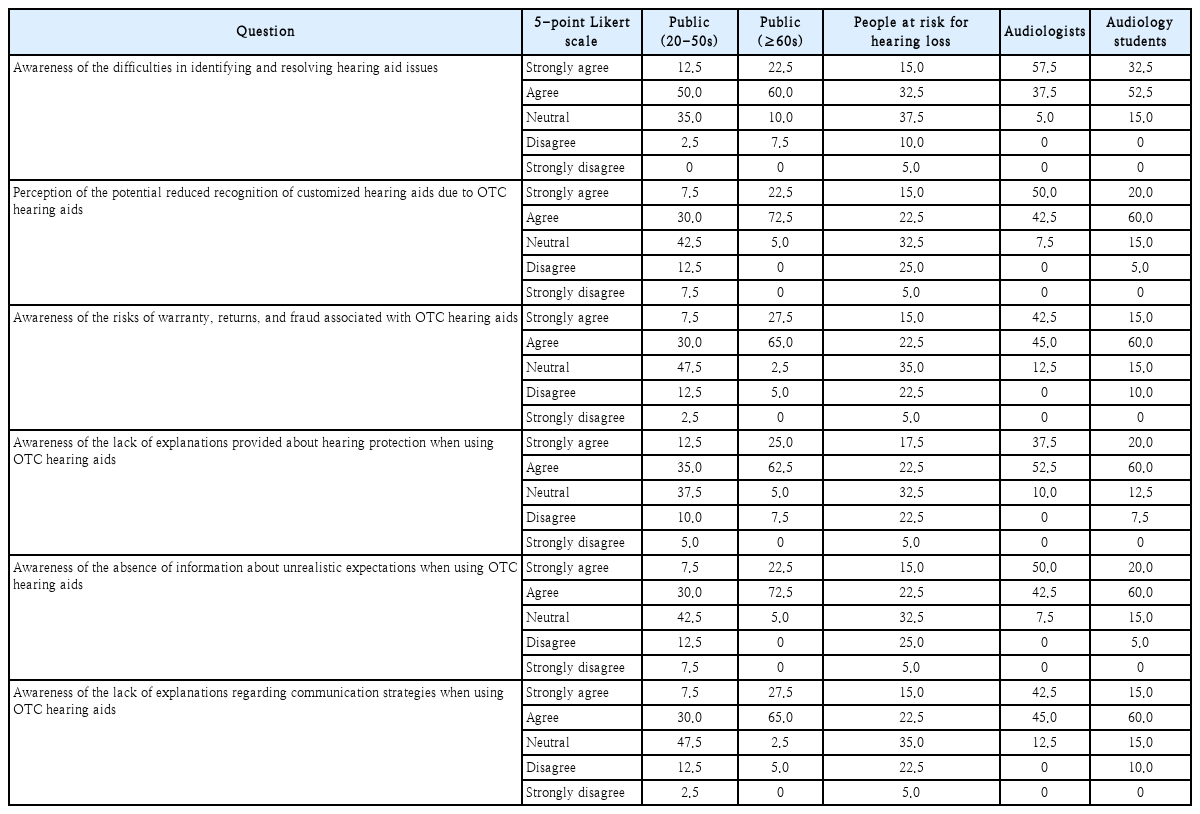
Based on responses summarized in Table 3, the professional groups (licensed audiologists and students) and the public aged 60 years and older generally showed very high levels of concern. For difficulty in identifying and resolving hearing aid problems, agreement (“strongly agree” and “agree”) was 95.0% in licensed audiologists, 85.0% in students, and 82.5% in the public aged 60 years and older. In licensed audiologists, “strongly agree” alone reached 57.5%. In contrast, agreement was relatively lower in the public aged 20 to 50 years (62.5%) and the at-risk group (47.5%), showing clear differences in perceptions of ability to resolve technical issues during actual use. For potential reduced recognition of customized hearing aids due to OTC hearing aids, agreement was high in older adults (95.0%) and licensed audiologists (92.5%), and students were also high at 80.0%. However, the public aged 20 to 50 years and the at-risk group each showed 37.5% agreement, indicating relatively low concern about the possibility that system expansion may reduce the perceived necessity and value of customized hearing aids.
For risks related to warranty, returns, and fraud, particularly strong concerns were observed in the public aged 60 years and older (92.5%) and licensed audiologists (87.5%), followed by students (75.0%). In contrast, agreement was lower in the public aged 20 to 50 years and the at-risk group (37.5%), and many neutral or non-agree responses were included in these groups.
Similar patterns were observed for the three items related to lack of counseling and education (Table 3). For awareness of the lack of explanations about hearing protection, agreement was 90.0% in licensed audiologists, 87.5% in the public aged 60 years and older, and 80.0% in students, whereas agreement was below half in the public aged 20 to 50 years (47.5%) and the at-risk group (40.0%). For awareness of the absence of information about unrealistic expectations, agreement was very high in the public aged 60 years and older (95.0%), licensed audiologists (92.5%), and students (80.0%), but low in the public aged 20 to 50 years and the at-risk group (37.5% each). For awareness of the lack of explanations regarding communication strategies, agreement was highest in the public aged 60 years and older (92.5%) and licensed audiologists (87.5%), and students (75.0%) were also high. These findings suggest that professionals and older adults strongly recognize the need for education on communication strategies to improve effectiveness in real listening situations, beyond simple instruction on device use..
In addition, chi-square tests conducted for all items in Table 3 showed that differences in response distributions across groups were all statistically highly significant (all items p<0.001). These values clearly support that perception gaps by age and expertise are prominent in all domains directly related to consumer protection, including problem solving, reduced recognition of customized value, warranty and fraud risk awareness, and lack of hearing protection and counseling education. Accordingly, when introducing OTC hearing aids, a group-tailored service and counseling system is needed, and hearing protection, expectation adjustment, and communication strategy education emphasized by professionals and older adults should be key strategies in policy design.
Expected efficacy and concern about adverse outcomes
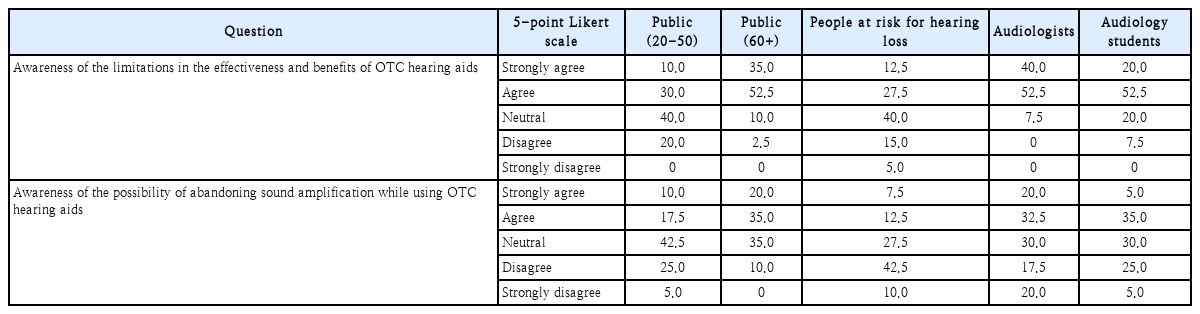
In Table 4, group differences in perceptions of OTC hearing aid efficacy were distinct. Specifically, statistical analysis of the item on awareness of limitations in effectiveness and benefits showed a highly significant group difference in response distribution (χ2=57.65, p=0.0000013). Licensed audiologists (92.5%) and the public aged 60 years and older (87.5%) strongly perceived that OTC hearing aids are less effective than conventional customized hearing aids, and many students (72.5%) also responded negatively. In contrast, in the public aged 20 to 50 years and the at-risk group, responses were more evenly distributed across agreement (40.0%), neutral (40.0%), and disagreement (20.0%).
For awareness of the possibility of abandoning sound amplification while using OTC hearing aids, a statistically significant group difference was also confirmed (χ2=34.79, p=0.0043). Concern about abandonment was greatest in the public aged 60 years and older (55.0%) and licensed audiologists (52.5%), and students showed evenly distributed agreement, neutral, and disagreement. The public aged 20 to 50 years had many neutral responses (42.5%). In the at-risk group, disagreement (52.5%) was higher than agreement (20.0%), indicating that the view that they would not abandon use was more prevalent. These findings show that statistically distinct differences in perception exist by age and expertise for both items. Professionals and older adults were skeptical about efficacy and perceived higher likelihood of abandonment, whereas younger adults and the at-risk group showed more diverse and neutral attitudes.
Additional question analysis in professional groups
In this study, licensed audiologists were analyzed as a clearly separated subgroup within professionals, and the survey results and tables consistently indicated that they reflect audiologists’ opinions. In licensed audiologists, about 60% showed a positive stance regarding expanded accessibility through OTC hearing aids, but 40% expressed concerns about effectiveness due to limitations of self-fitting and difficulty addressing severe hearing loss. For expectations about market activation, positive (45%) and negative (55%) responses were similar, and lack of professional examination and insufficient consumer education were identified as hindering factors. Willingness to recommend OTC hearing aids was very low (2.5%), and audiologists emphasized the importance of customized hearing aids and professional management. For the possibility of implementation, 72.5% responded that it was high.
Among audiology students, 70% had no education experience related to OTC hearing aids, and 85% evaluated the possibility of national implementation as high. Concern about negative impacts of OTC hearing aids on audiology professions (52.5%) and vigilance regarding technical limitations were also high. Although 82.5% responded that OTC hearing aids would increase accessibility for individuals with hearing loss, 72.5% responded that they would not recommend them to acquaintances, suggesting low intention to recommend and use for themselves and people around them. In addition, most (90%) responded that they recommend customized hearing aids to acquaintances.
Discussion
This study compared and analyzed perceptions, concerns, and expectations regarding the OTC hearing aid system, which has not yet been officially implemented in Korea, among diverse groups including the general public, individuals at risk for hearing loss, licensed audiologists, and students. As OTC hearing aid systems have been introduced in some developed countries including the United States, discussions of similar system introduction have begun in Korea. However, there are few empirical studies on actual acceptability and expectations and concerns among various stakeholders [8,11]. The significance of this study lies in its systematic examination of group-specific patterns of perceptions and concerns in the Korean context prior to system introduction, providing realistic foundational data for future policy establishment.
Group differences in acceptability and information needs
Information needs and acceptance attitudes regarding OTC hearing aids differed clearly by age and expertise. In the public aged 20 to 50 years, only about half were interested in information, and the at-risk group was passive in acquiring information. This again confirms that, as reported by Reed, et al.,4) even among individuals with hearing loss, key reasons for low access or interest in hearing aids include lack of self-awareness and psychological barriers to device use. Meanwhile, licensed audiologists and students were active in obtaining information and showed high agreement regarding counseling competence and the need for workplace education, indicating a sense of responsibility in professional groups and an intention to build at least minimal information networks. Prior studies conducted in the United States and elsewhere also emphasize that strengthening professional education and consumer counseling systems is a key issue when OTC systems are introduced [7,11].
Practical and cognitive barriers related to self-insertion and self-adjustment
Practical success in OTC hearing aid use depends on how easily consumers can perform self-fitting processes such as self-insertion and sound adjustment. In this study, concerns about difficulty of self-insertion and adjustment were very high in older adults aged 60 years and older and in professional groups. This is consistent with findings from Boothroyd and Mackersie [12] and Convery, et al. [13], which suggest that operational failures and fitting errors occur frequently in early use stages. Younger adults and the at-risk group showed neutral or lower concern, but this may reflect perceptions prior to actual experience. Therefore, for the system advantage of accessibility to translate into real effectiveness and sustained use at the usage stage, tailored education for older consumers, product design centered on ease of use, and technical support should be prerequisites [14].
Service and counseling gaps and consumer protection concerns
The most prominent common concerns in this study were after-sales service (A/S), quality degradation due to lack of counseling, and risk of harm. Licensed audiologists and students expressed concerns in all domains such as consumers’ ability to solve problems independently, insufficient warranty, undermining of recognition of customized hearing aids, and inappropriate expectation setting, with high concern levels above 80%. This suggests that, as noted by Convery, et al. [13] and Almufarrij, et al. [7], excluding systematic counseling and fitting processes may increase vulnerability to fitting errors, risks of underamplification and overamplification, and increased returns and fraud. Older adults also expressed strong anxiety about lack of professional involvement. In contrast, younger adults and the at-risk group were relatively neutral. However, in Korea, actual OTC usage experience is still limited, and a structured system should be established in advance given that service and counseling demand may increase sharply upon commercialization [11].
Group perceptions on efficacy, expectations, and risk of abandonment
Most professionals and older adults considered OTC hearing aids less effective than professionally fitted hearing aids. This aligns with randomized clinical trials by De Sousa, et al. [15] and findings by Keidser, et al. [16], which repeatedly confirm differences in listening outcomes and adaptation satisfaction between self-fitting and professional fitting groups. In addition, the risk of abandoning hearing aid use was much higher among professionals and older adults, whereas confidence was higher in the at-risk group, but the possibility of short-term self-report cannot be excluded. Therefore, long-term follow-up studies are needed in the future.
Additional views among professionals and students
Although 60% of licensed audiologists evaluated OTC hearing aids as helpful for improving market accessibility, 40% were highly concerned about limitations of self-fitting, inability to address severe hearing loss, and risks due to insufficient quality assurance. Expectations about the prospect of national activation were split between positive (45%) and negative (55%), and consumer education, exchange and A/S systems, and fitting manual education systems were identified as key variables determining system effectiveness. In practice, professional groups showed markedly low willingness to recommend OTC hearing aids to acquaintances (2.5% to 10%), and students reported substantial occupational concerns. This is consistent with recent research trends emphasizing the importance of existing professional-centered service models and direct in-person management [11,17].
Study limitations and directions for future research
This study is meaningful in that it assessed attitude and perception structures through definition explanation and survey in the Korean context where OTC hearing aids have not yet been implemented. However, several limitations are evident. First, opinions from some critical stakeholders such as otorhinolaryngologists were not sufficiently reflected. In the early stage, it was judged that licensed audiologists and audiology students were most closely linked to OTC hearing aid markets and policy trends, and thus the sample was composed accordingly. Excluding various professional roles such as otorhinolaryngologists remains a major limitation. This may restrict discussion on the need for professional involvement and medical diagnostic systems, and future studies should emphasize sufficient participation of otorhinolaryngologists and collection of multifaceted opinions. Second, about 40% of the sample consisted of licensed audiologists and students, indicating occupational overrepresentation. In addition, exogenous variables such as region, centered on the metropolitan area, and digital literacy were not sufficiently controlled in the sampling process. Although the sample size was statistically sufficient, cautiou is needed when considering representativeness and generalizability. Third, because this study did not include actual OTC hearing aid users, it could not quantitatively analyze problems or expectation-experience gaps based on real-world use. Fourth, given the self-report nature of surveys, social desirability bias may be present, and caution is required in interpretation.
Future studies should include actual OTC hearing aid users and conduct longitudinal studies, compare real-world clinical utility, and verify effectiveness of digital accessibility education programs. In addition, as technology evolves, multilayered evaluations of app-based self-fitting and monitoring, and development of shared professional and public models within service and counseling systems, should be studied as realistic alternatives for system establishment.
In conclusion, this study empirically confirmed that major expectations and concerns associated with OTC hearing aid system introduction, improved accessibility alongside quality degradation and increased vulnerability in consumer protection, coexist in practice. For successful policy implementation and market introduction, multilayered protective measures are essential, including consumer education, linkage to professional examination, and user-tailored technical guidance.
Supplementary Materials
Korean translation of this article is available with the Online-only Data Supplement at https://doi.org/10.3342/kjorl-hns.2025.00451.
The Supplement is available with this article at https://doi.org/10.3342/kjorl-hns.2025.00451.
Notes
Acknowledgments
This work was supported by the Ministry of Education of the Republic of Korea and the National Research Foundation of Korea (NRF-2022S1A5C2A03091539).
Author Contribution
Conceptualization: Woojae Han. Data curation: Jieun Joo, Ayoung Lee, Jieun Eom, Minsik Park, Hanseul Park. Funding acquisition: Woojae Han. Methodology: Jieun Joo, Hanseul Park. Writing—original draft: Jieun Joo, Woojae Han. Writing—review & editing: all authors.