A Case of Tuberculous Otitis Media Diagnosed Before Surgery and Treated Successfully With Anti-Tuberculosis Medication
수술 전 진단으로 항결핵제 치료만으로 호전된 결핵성 중이염 1예
Article information
Abstract
Tuberculous otitis media (TOM) is a rare form of chronic otitis media that often exhibits atypical characteristics and is challenging to diagnose. We report the case of a 35-year-old man with 6 months of persistent otorrhea, aural fullness, and hearing loss that did not respond to antibiotic treatment. Otoscopy showed a thickened and retracted tympanic membrane without perforation, and temporal bone computed tomography revealed soft tissue density in the middle ear and mastoid. Although the middle ear biopsy was inconclusive, pulmonary lesions were detected on chest imaging, and Mycobacterium tuberculosis was confirmed by polymerase chain reaction from bronchoalveolar lavage. The patient was diagnosed with TOM associated with pulmonary tuberculosis and treated with standard anti-tuberculosis medication, resulting in resolution of otorrhea, improvement of hearing, and no recurrence at 18 months. This case highlights the importance of considering TOM in refractory otitis media and shows that early suspicion can enable successful medical treatment without surgery.
Introduction
Tuberculous otitis media (TOM) is a rare form of chronic otitis media caused by Mycobacterium tuberculosis, and it has been reported in 0.04% to 0.9% of patients with chronic otitis media [1]. Compared with the past when the prevalence of tuberculosis was high, the incidence of TOM has decreased after the widespread use of anti-tuberculosis medications and the introduction of tuberculosis control strategies [2]. Nevertheless, TOM remains a significant clinical challenge in the otologic field due to the frequent delay in diagnosis.
The typical clinical features of TOM include otorrhea, multiple tympanic membrane perforations, hearing loss, granulation tissue formation, and a course that does not respond to antibiotics. In some patients, facial nerve palsy or temporal bone destruction may also be present [3]. In actual clinical practice, however, it is uncommon for all these typical characteristics to appear, and many cases present with atypical features and may be mistaken for simple chronic otitis media, fungal infection, or neoplastic lesions. For this reason, diagnosis is often delayed, and many patients are confirmed only by pathologic examination after surgical treatment.
For early diagnosis of TOM, it is important to consider not only clinical symptoms and physical findings but also the patient’s history of tuberculosis exposure, the presence of tuberculosis in other sites, such as pulmonary tuberculosis or tuberculous lymphadenitis, and the use of microbiologic and molecular diagnostic tests. Early diagnosis can lead to positive outcomes with anti-tuberculosis medication alone, allowing unnecessary surgical procedures to be avoided. The authors experienced a case of TOM, presumed to be accompanied by pulmonary tuberculosis, in a patient with chronic otitis media showing an atypical course, which improved with anti-tuberculosis medication alone without surgery or complications, and we report this case with a review of the literature.
Case
A 35-year-old man presented with left otorrhea persisting for 6 months. He had received antibiotic treatment at another hospital for 6 months under a diagnosis of chronic otitis media, but symptoms persisted, and he visited our hospital. Left ear discomfort began after he blew his nose strongly, following mild cold symptoms such as cough and sputum. In addition to otorrhea, he had aural fullness and hearing loss, and there were no findings of dizziness or facial palsy. Endoscopic examination showed left purulent otorrhea, and the tympanic membrane showed erythema and opacity with retraction, but no perforation was observed (Fig. 1A). Gram staining of the otorrhea showed a small amount of Gram-positive cocci, and bacterial culture identified Staphylococcus epidermidis. Pure-tone audiometry showed a left bone-conduction threshold of 16 dB and an air-conduction threshold of 40 dB, and the right ear had normal hearing (Fig. 2A). Temporal bone CT showed the presence of soft tissue density within the left middle ear cavity and mastoid, with no evidence of bony erosion, including the ossicles (Fig. 3A). Blood testing showed no specific findings except a mild elevation of C-reactive protein to 0.62 mg/dL. Prior to planning surgical treatment, an exploratory myringotomy was performed for an accurate diagnosis, including confirmation of the middle ear lesion. Granulation tissue filled the middle ear cavity, and pathologic examination was performed with a small amount of sampled tissue, but it showed only chronic inflammation.
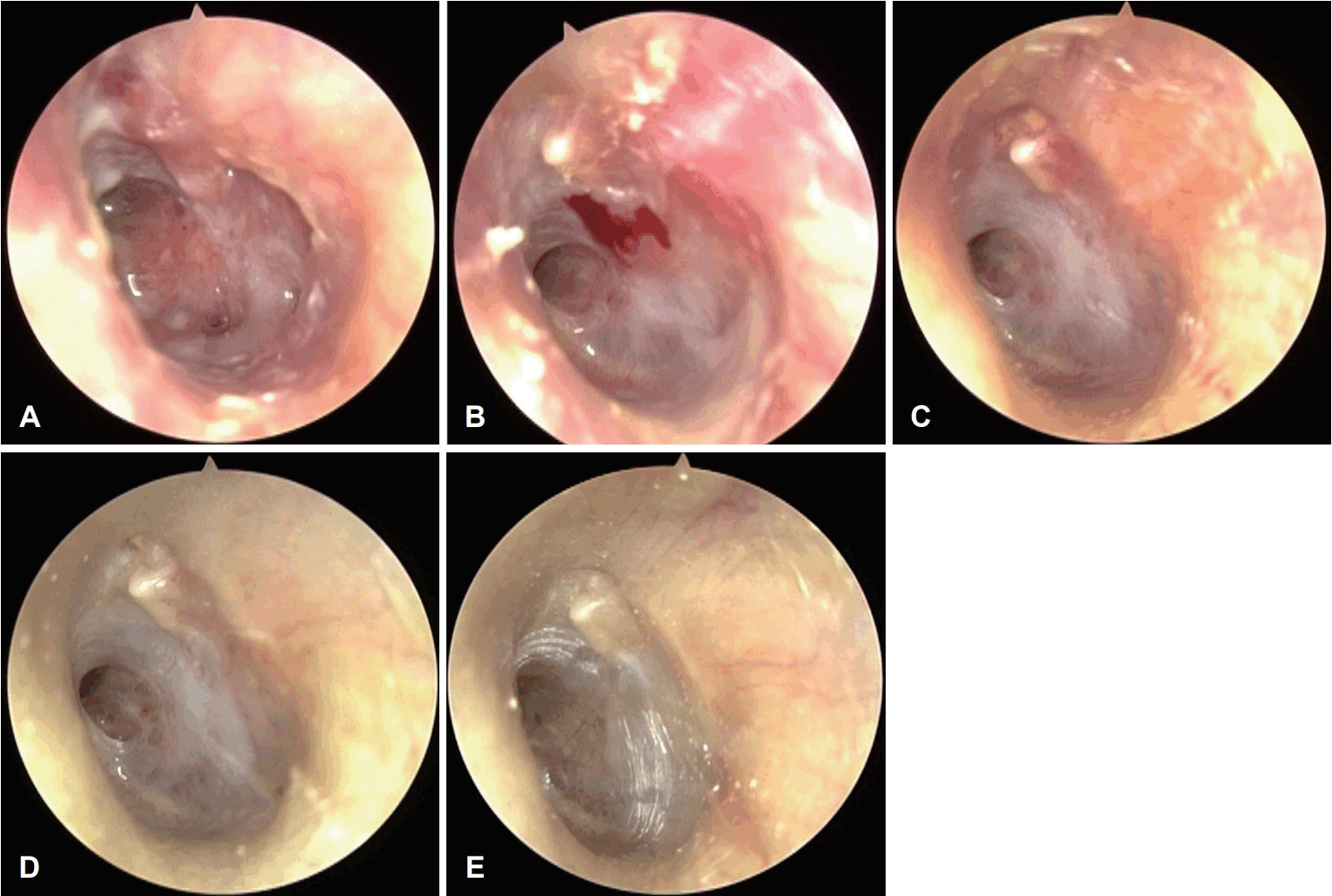
Serial endoscopic findings. A: At initial presentation, the tympanic membrane showed diffuse hyperemia, thickening, and retraction without perforation. B: At 2 months of anti-tuberculosis treatment, erythema and thickening have decreased, and the granulation tissue has partially resolved. C: At 4 months, the tympanic membrane demonstrated further resolution of granulation with improvement in aeration of middle ear. D: At the end of 6 months of anti-tuberculosis treatment, the tympanic membrane showed near-complete resolution with restored middle ear aeration, although mild retraction around the eustachian tube orifice remained. E: At 18 months after treatment, the tympanic membrane remained intact without recurrence.
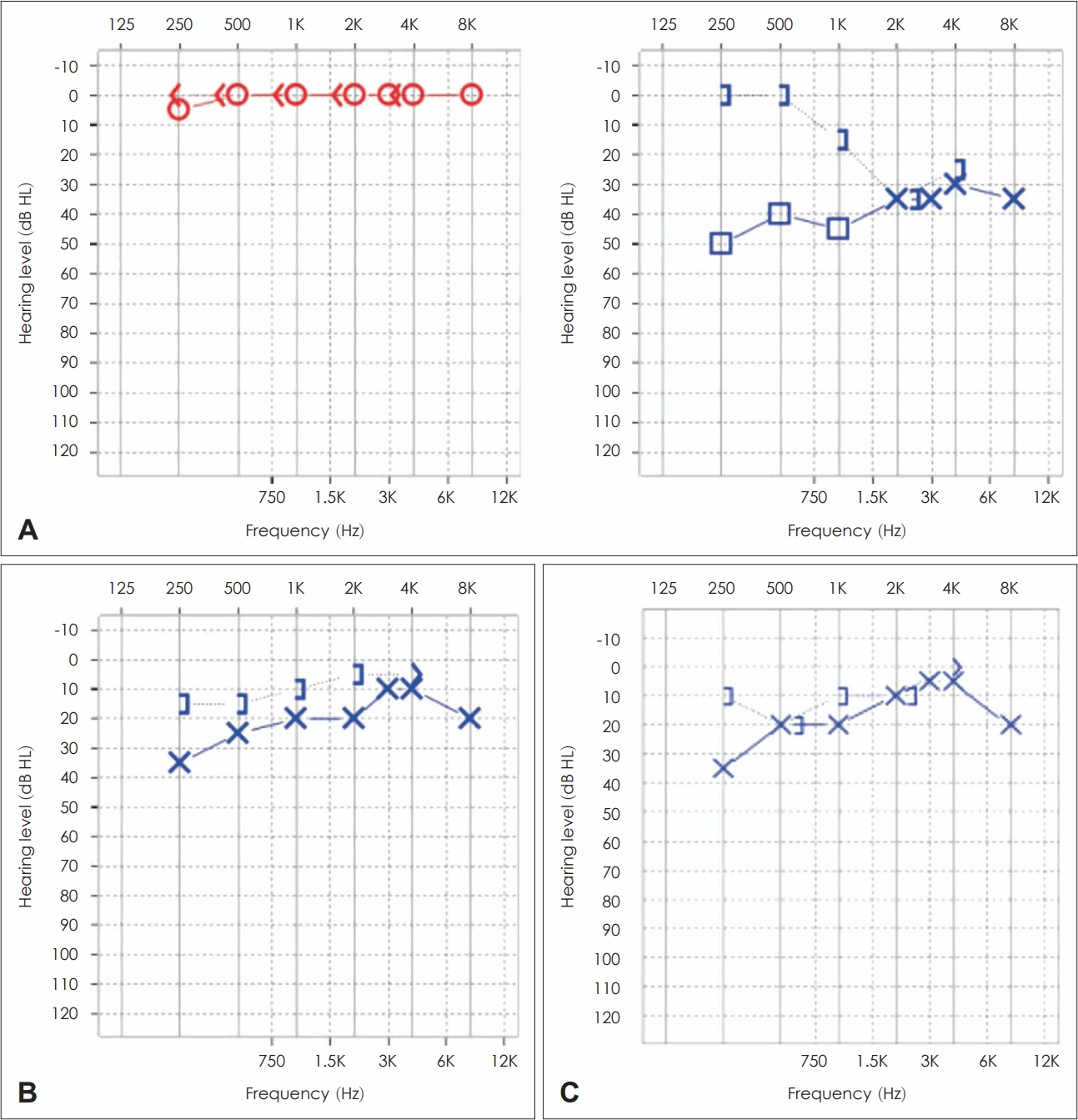
Serial results of pure-tone audiometry. A: At initial presentation, conductive hearing loss was noted in the left ear. B: At the end of anti-tuberculosis treatment (6 months), the air-bone gap had improved. C: At 18 months follow-up, hearing remained stable with near-complete closure of the air-bone gap.
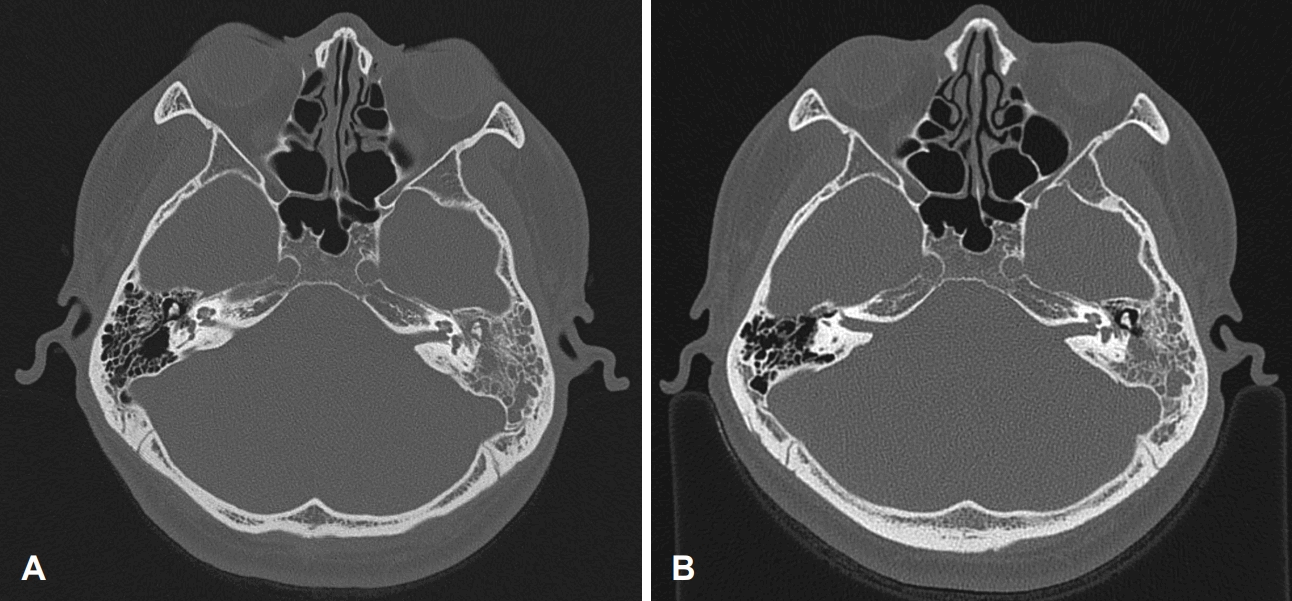
Temporal bone computed tomography (CT) findings. A: At initial presentation, CT scan showed soft tissue density filling the middle ear cavity and mastoid air cells without definite bony destruction. B: At 18 months after anti-tuberculosis treatment, CT demonstrated resolution of soft tissue density in the middle ear cavity, with residual soft tissue density in the mastoid.
The patient was hospitalized and treated with intravenous antibiotics, but there was no improvement. On the chest radiograph obtained at admission, multiple irregular hazy opacities were observed in both upper lung fields, raising suspicion for tuberculosis infection. An additional low-dose chest CT also confirmed multiple clustered centrilobular nodules in both lungs, and active tuberculosis with a bronchogenic spread pattern was considered highly likely. Sputum testing and bronchoscopy were performed to differentiate pulmonary tuberculosis. Using sputum and bronchoalveolar lavage fluid as specimens, acid-fast bacilli smear and culture, Mycobacterium tuberculosis polymerase chain reaction (PCR), potassium hydroxide (KOH) test, fungal culture, and cytopathologic examination were performed. In addition, a small amount of granulation tissue from the middle ear cavity was additionally obtained, and Mycobacterium tuberculosis PCR was performed. Among the results from various specimens, only the Mycobacterium tuberculosis PCR from bronchoalveolar lavage fluid was positive, and the subsequently reported interferon-gamma release assay result was positive.
With a diagnosis of TOM accompanied by pulmonary tuberculosis, standard 6-month anti-tuberculosis medication was initiated, consisting of a 2-month intensive phase including isoniazide, rifampin, ethambutol, and pyrazinamide, followed by a 4-month continuation phase including isoniazide and rifampin. At 2 months after treatment initiation, otorrhea and granulation tissue of the tympanic membrane improved, but tympanic membrane opacity and retraction persisted (Fig. 1B). At 4 months, tympanic membrane opacity and retraction showed improvement, but retraction around the opening of the Eustachian tube in the anterior superior tympanic membrane remained (Fig. 1C). After 6 months of anti-tuberculosis medication, middle ear aeration appeared complete, and only retraction around the Eustachian tube orifice persisted (Fig. 1D). Pure-tone audiometry showed a left bone-conduction threshold of 10 dB and an air-conduction threshold of 21 dB, leaving an air-bone gap of about 10 dB (Fig. 2B). At 1 year and 6 months after treatment initiation, tympanic membrane findings showed additional improvement of the remaining retraction around the Eustachian tube orifice (Fig. 1E). Temporal bone CT showed complete resolution of soft tissue density in the middle ear cavity, but residual findings were still observed in the mastoid (Fig. 3B). Pure-tone audiometry showed a left bone-conduction threshold of 13 dB and an air-conduction threshold of 16 dB, and the patient had no subjective discomfort (Fig. 2C).
Discussion
TOM is not easy to diagnose in actual clinical practice because of its low prevalence and diverse clinical presentations. As a result, unnecessary surgical treatment may be performed, or complications may occur because improvement is not achieved despite prolonged antibiotic treatment.
The known routes of infection in TOM include direct spread through the Eustachian tube of Mycobacterium tuberculosis present in sputum in patients with pulmonary tuberculosis, hematogenous spread to the temporal bone from systemic tuberculosis foci, and direct spread through the external auditory canal or a perforated tympanic membrane [4]. In this case, based on the history that otorrhea, aural fullness, and hearing loss began after forceful nose blowing during mild cold symptoms, this suggests the possibility that Mycobacterium tuberculosis penetrated into the middle ear cavity through the Eustachian tube.
The most significant diagnostic challenge associated with TOM is that it is difficult to diagnose until it is suspected. Characteristic clinical findings have been reported, such as painless otorrhea, multiple perforations, and pale granulation tissue filling the middle ear cavity. However, diagnosis is difficult because such characteristic findings rarely appear, depending on the disease course. In addition, even when testing is performed after suspicion, the positive rate of acid-fast bacilli staining using specimens obtained from the middle ear cavity is reported to be about 5% to 35%, and the positive rate of culture is about 20% to 40%, which are very low [5]. Although the positive rate of Mycobacterium tuberculosis PCR is reported to be about 81.6%, which is relatively high compared with other confirmatory tests [6], PCR from the middle ear cavity specimen can also be reported as negative as in this case. The reasons for these false-negative results are reported to include a low concentration and non-uniform distribution of Mycobacterium tuberculosis within tissue in TOM, and inhibition of PCR reactions by coexisting blood [3,7]. Therefore, in primary TOM without accompanying tuberculosis in other organs, the final diagnosis is mostly made using specimens obtained through a surgical approach. This case was secondary TOM with suspected pulmonary tuberculosis, and confirmation was possible using the bronchoalveolar lavage fluid specimen. If not, it is highly likely that surgery for diagnostic and therapeutic purposes would have been performed.
Early diagnosis and treatment are important in TOM, and when pulmonary tuberculosis is accompanied, anti-tuberculosis medication is the principle. However, when complications such as facial nerve palsy, meningitis, subperiosteal abscess, labyrinthitis, or similar conditions are accompanied, surgical treatment is performed first, and then anti-tuberculosis medication is started [8,9]. In this case, by suspecting TOM early before progression to complications, treatment was possible with medication alone, and unnecessary surgical treatment could be avoided.
Through this case, the improvement course of TOM after anti-tuberculosis medication could be observed. According to previous reports, anti-tuberculosis medication can lead to disappearance of otorrhea and suppression of granulation tissue growth within several weeks [10], and improvement of hearing and middle ear ventilation is often fully observed at the time of completion of 6 months of medical treatment [11,12]. In this patient as well, findings indicated that granulation tissue formation was suppressed after 1 month of treatment, and hearing and tympanic membrane findings clearly recovered at 6 months. During follow-up phase of treatment, it is essential to closely monitor changes in otorrhea and granulation tissue, the recovery of tympanic membrane aeration, and any hearing changes. Because clinical improvement often precedes radiologic changes in TOM, regular temporal bone CT is not recommended. It is desirable to perform CT selectively only when clinical improvement is insufficient, when recurrence or complications are suspected, or when surgical intervention should be considered [13]. In this case, temporal bone CT after completion of treatment showed the disappearance of soft tissue density in the middle ear cavity, but some density remained in the mastoid. According to previous reports, such residual density is more often interpreted as scar tissue or fibrosis rather than progressive infection, and if there is no evidence of bony erosion and the patient is asymptomatic, additional surgical intervention is not necessary [14,15]. In this case as well, the patient remained stable without recurrence or complications during 18 months of follow-up.
TOM is challenging to diagnose due to its low prevalence and atypical clinical presentations. Nevertheless, the most critical point is to diagnose early and initiate treatment. Therefore, in cases of chronic otorrhea that do not respond to antibiotics or when granulation tissue is observed, the possibility of TOM should be considered. This case involved a patient with accompanying pulmonary tuberculosis in whom TOM was suspected before surgery, and improvement was confirmed with anti-tuberculosis medication alone. Although there was a limitation in that Mycobacterium tuberculosis could not be directly confirmed from the middle ear specimen, TOM could be judged by integrating the accompanying findings of pulmonary tuberculosis and the pattern of clinical improvement with anti-tuberculosis medication. Consequently, unnecessary surgery was avoided, and early treatment was possible before complications occurred, and the healing process could be closely followed while treating with anti-tuberculosis drugs.
Supplementary Materials
Korean translation of this article is available with the Online-only Data Supplement at https://doi.org/10.3342/kjorl-hns.2025.00465.
Notes
Acknowledgments
None
Author Contribution
Conceptualization: Jungmin Ahn. Data curation: Changhoon Kwon. Investigation: Seong-Eun Hong. Supervision: Jungmin Ahn. Visualization: Seong-Eun Hong. Writing—original draft: Changhoon Kwon. Writing—review & editing: Jungmin Ahn.
