Retroauricular Revolving Door Island Flap for Auricular Basal Cell Carcinoma
이개 기저세포암에서 후이개 회전문 섬피판술을 이용한 재건
Article information
Abstract
Auricular reconstruction, particularly of the conchal bowl, remains a significant surgical challenge because of the region’s complex anatomy and high aesthetic and functional demands. We report cases of basal cell carcinoma involving the conchal bowl and the external auditory canal (EAC) that were successfully reconstructed using the single-stage retroauricular revolving door island flap (RDIF) technique. In these patients, the flaps demonstrated complete viability without major complications such as necrosis, infection, or canal stenosis. The reconstructed auricles preserved their natural contour with excellent cosmetic outcomes, and functional results were satisfactory. These cases highlight the RDIF technique as a reliable, versatile, and effective option for the reconstruction of moderate-sized conchal and EAC defects, providing excellent aesthetic and functional outcomes in a single stage.
Introduction
Basal cell carcinoma (BCC) is the most frequent malignant tumor of the external ear, especially in chronically sun-exposed regions such as the auricular concha [1]. Complete excision with tumor-free margins remains the mainstay of treatment. However, defects involving the conchal bowl and external auditory canal (EAC) pose unique reconstructive challenges: the skin is thin and tightly adherent to cartilage, donor site availability is limited, and both aesthetic and functional preservation (particularly canal patency) are essential [2].
Traditional reconstructive options include secondary intention healing, skin grafts, and interpolation flaps. Secondary intention can be suitable for small superficial defects but risks contraction and prolonged healing time. Skin grafts are prone to shrinkage, contour deformity, and poor color match, and are less effective when cartilage is removed [3]. Interpolation flaps achieve durable coverage but require multiple stages and leave conspicuous donor scars [4].
The retroauricular revolving door island flap (RDIF), first described by Masson [5] in 1972, is a single-stage local flap harvested from the retroauricular and mastoid skin. It is pedicled on the subcutaneous tissue in the retroauricular groove, which is richly supplied by an anastomotic arcade between the posterior auricular and superficial temporal arteries [6]. The flap rotates through a cartilage window like the wings of a “revolving door,” resurfacing the anterior auricular defect while leaving the donor site hidden posteriorly [7]. Reported advantages include reliable vascularity, excellent contour and color match, concealed donor site, and preservation of EAC lumen [8].
This report describes two patients with auricular BCC involving the conchal bowl, reconstructed successfully with the RDIF technique (Fig. 1).
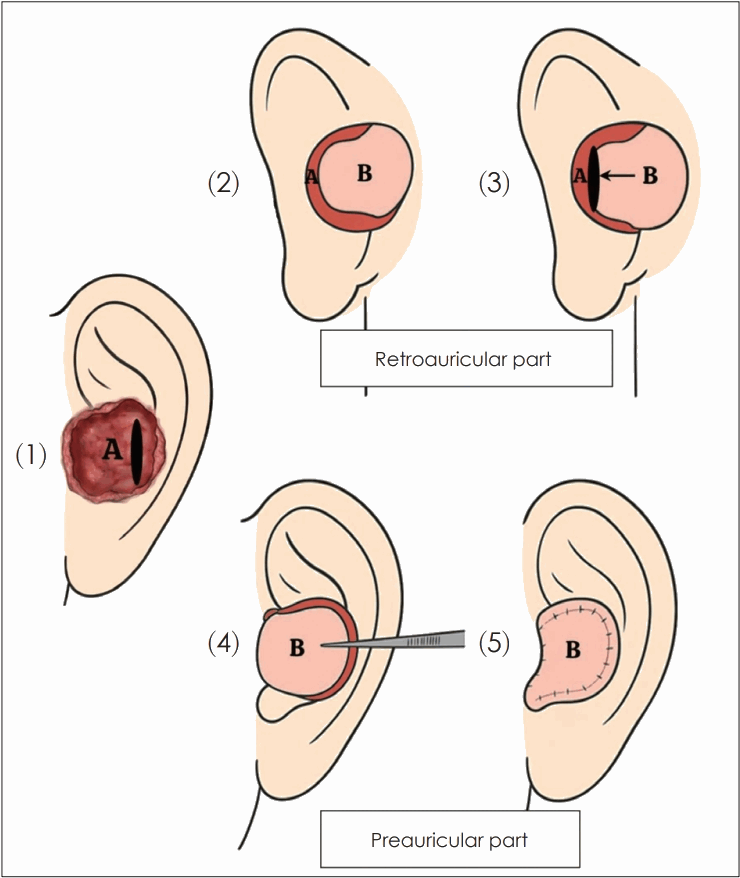
Schematic illustration of the retroauricular revolving door island flap technique. The defect is depicted in pale red (A) and the flap in apricot (B). (1) Preauricular view showing the defect (A) and the cartilage window. (2) Retroauricular view showing the design of the island flap (B). (3) Transposition of the flap (B) anteriorly through the cartilage window. (4) Preauricular view showing the flap (B) rotated to cover the defect. (5) Final postoperative appearance after suturing.
Cases
Case 1
An 88-year-old female patient with a medical history of mild cardiomegaly and angina presented to our hospital with complaints of pain in the right ear for several weeks. Physical examination revealed an irregularly elevated, slightly ulcerated lesion involving the right conchal bowl and extending to the EAC inlet. The conchal mass measured approximately 1.5×1.5 cm, and a smaller, 0.5×0.5 cm tumor was noted at the EAC entrance; both lesions were connected (Fig. 2A). A punch biopsy performed at an outside hospital revealed BCC, adenoid type.
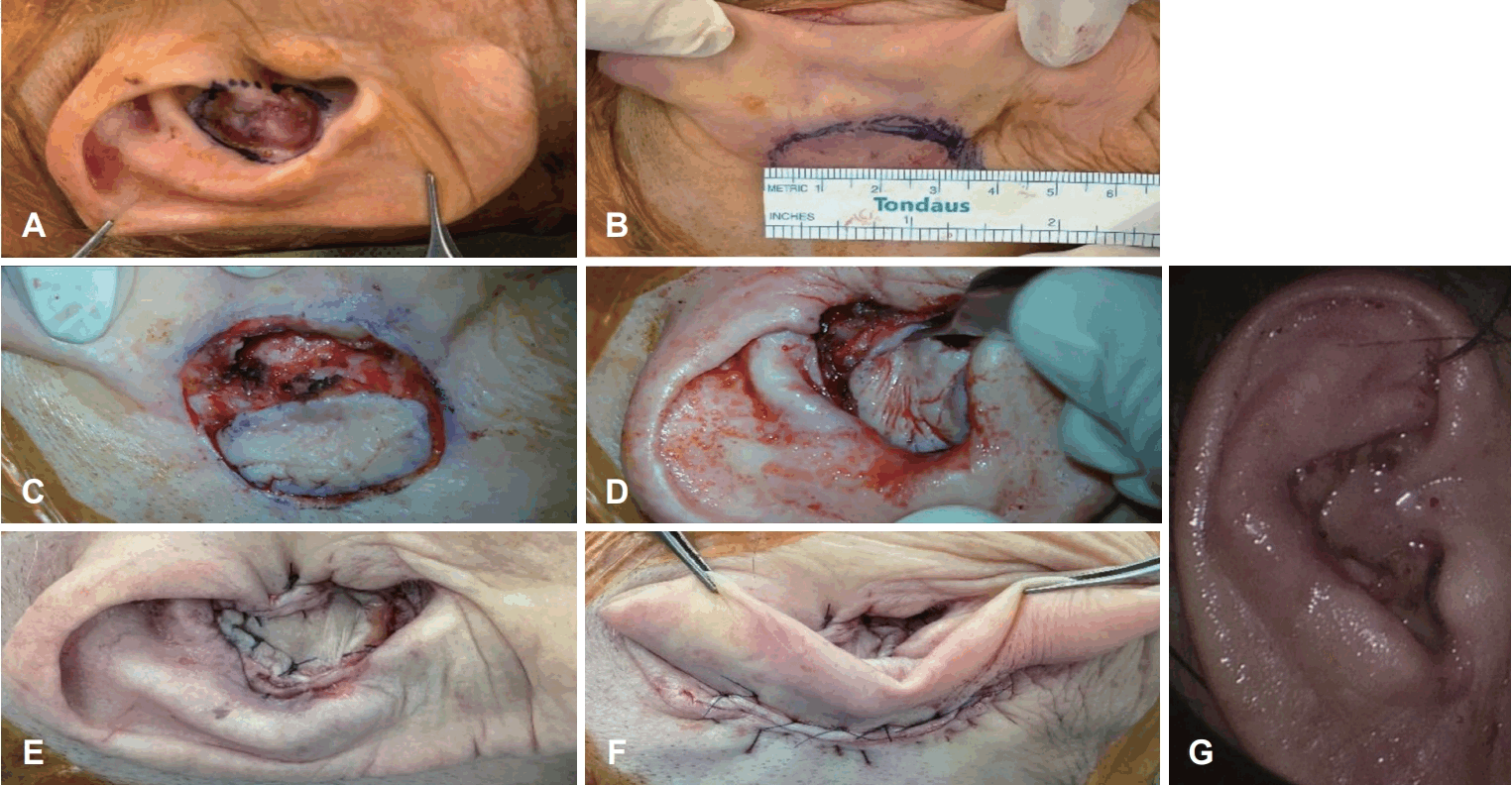
Surgical procedure and clinical outcome for Case 1. A: Connected conchal masses noted at the Rt. EAC entrance. B: Preoperative design of the wide local excision including the auricular cartilage. C and D: Intraoperative photographs demonstrating the elevation and transposition of the retroauricular RDIF. E and F: Postoperative view of the conchal bowl after reconstruction. G: Two-week postoperative appearance demonstrating a well-healed flap without complications. EAC, external auditory canal; RDIF, revolving door island flap.
Preoperative workups, which were performed at an outside hospital, included neck CT and positron emission tomography-CT (PET-CT), which showed no evidence of lymph node or distant metastasis.
Surgical excision was performed under local anesthesia with lidocaine with 1:100000 epinephrine. After sterile preparation and draping, the excision was performed under microscopic visualization to ensure precise oncologic margins while preserving the healthy portion of the auricular cartilage. A wide local excision including the underlying auricular cartilage was performed, ensuring an oncologic safety margin of approximately 2 mm around the lesion (Fig. 2B). The excised specimen measured 2.5×2.2×1.1 cm in greatest dimension, consistent with the preoperative assessment. Hemostasis was achieved, and a retroauricular skin island flap was designed over the postauricular region. The flap was elevated with preservation of the central subcutaneous pedicle and rotated anteriorly through the cartilaginous defect, following the “revolving door” principle to cover the conchal and EAC defect (Fig. 2C and D). To eliminate dead space and prevent seroma formation, several anchoring sutures were placed between the undersurface of the flap and the conchal cartilage, similar to the tacking sutures used in pectoralis major flaps. The flap was secured using vertical mattress sutures with Vicryl for the supporting layer, rapid Vicryl for the subcutaneous layer, and nylon for the skin closure (Fig. 2E and F).
Postoperatively, the wound healed without complications, and the flap remained fully viable with no evidence of congestion, infection, or necrosis. The EAC lumen was well preserved without canal stenosis. Final histopathological examination confirmed BCC, adenoid type, with no lympho-vascular or perineural invasion. The lateral and deep margins were free of carcinoma, each with a 2-mm safety margin. Immuno-histochemical staining showed positivity for p63 and EpCAM, and negativity for EMA and CK7, consistent with a basaloid epithelial neoplasm.
At the 2-month follow-up, the flap maintained excellent color and contour matched with the surrounding tissue, and the auricular shape was well preserved without recurrence (Fig. 2G).
Case 2
A 53-year-old female patient visited our hospital for evaluation of a persistent lesion in the left EAC. She had experienced the pain and discomfort approximately 1-2 years prior. A punch biopsy performed at an outside hospital revealed a keratinocytic neoplasm suggestive of BCC, measuring approximately 0.5 cm in size with a depth of invasion of 0.4 cm (at least Clark level IV). No bone invasion, vascular invasion, or perineural invasion was identified. A second biopsy and excision were performed with adequate oncologic margins reportedly; however, the possibility of residual or recurrent disease could not be excluded. Therefore, the patient was referred to our hospital for further management and reconstruction.
Preoperative workups performed at an outside hospital included neck CT and PET-CT, which showed no evidence of lymph node or distant metastasis. Also, temporal bone MRI confirmed that the lesion was confined to the auricular cartilage and superficial EAC without invasion of cerebellopontine angle cistern and internal auditory canal.
Surgical excision of left EAC tumor was performed under local anesthesia. To ensure precise tumor removal and cartilage preservation in the narrow EAC, the procedure was conducted under microscopic visualization. The previously biopsied area in the left inferior EAC and conchal region was identified. The EAC skin and a portion of the underlying cartilage were excised en bloc, opening the excision area to the retroauricular subcutaneous tissue. The excised specimen measured 1.5×1.1×0.5 cm in greatest dimension, which closely corresponded to the size estimated on preoperative measurement. A circular retroauricular flap (1.5×1.5 cm) was designed and elevated (Fig. 3A and B). The flap was rotated anteriorly through the defect using the “revolving door” technique and secured with vertical mattress sutures using Vicryl and rapid Vicryl for the subcutaneous layers, and 4-0 Nylon for the skin closure. To promote tissue adhesion and hemostasis, fibrin sealant (Tisseel) was applied to the flap bed prior to final closure. Also, a Merocel pack was inserted into the EAC to maintain patency and prevent canal stenosis, and Vaseline gauze was packed over the conchal bowl as a bolster dressing.
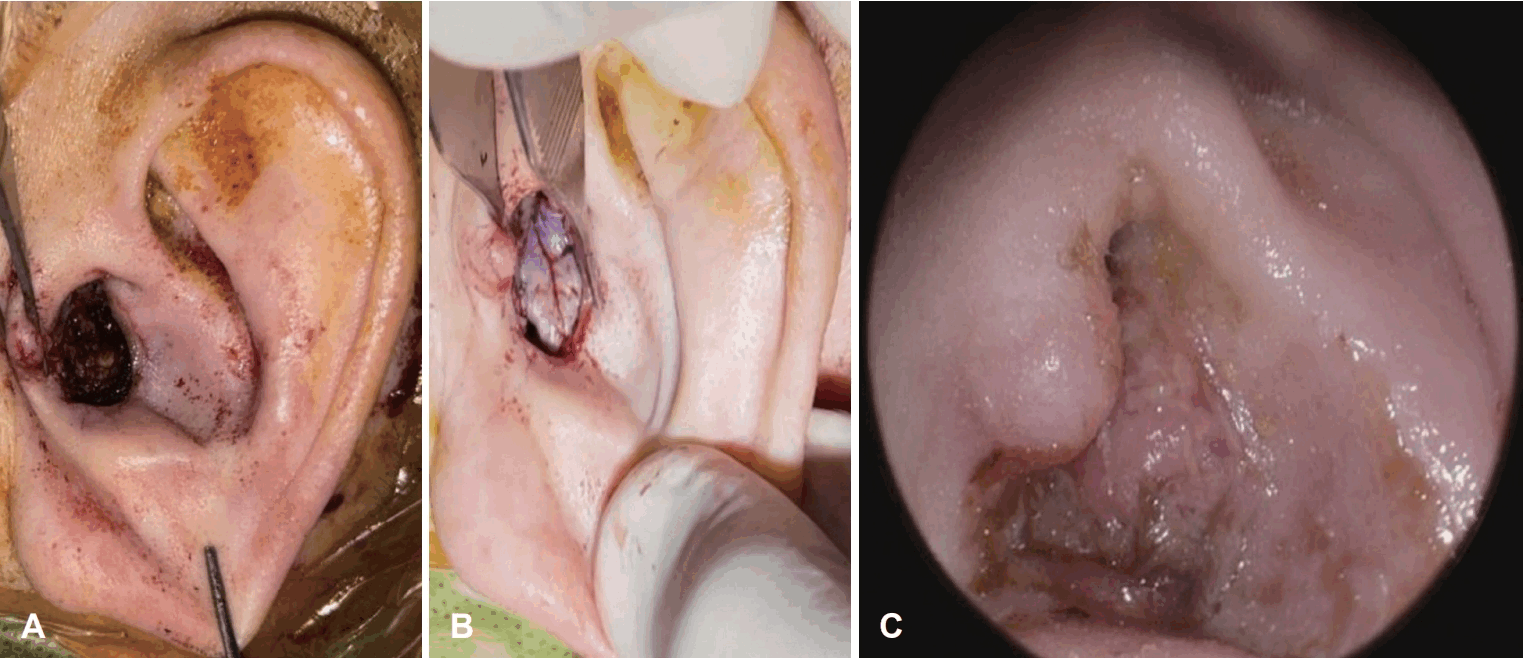
Surgical procedure and clinical outcome for Case 2. A: Intraoperative view of the conchal bowl and EAC defect after tumor excision. B: Reconstruction using the retroauricular RDIF. C: Postoperative appearance at 2 weeks showing a well-maintained EAC lumen without stenosis. EAC, external auditory canal; RDIF, revolving door island flap.
The postoperative course was uneventful. There were no signs of bleeding, infection, or flap congestion. The patient was discharged after regular dressing and wound inspection. Final pathological examination of the specimen showed no residual carcinoma, only granulation tissue formation consistent with a post-biopsy (at an outside hospital) healing process. All circumferential margins were free of carcinoma.
At follow-up, the flap remained viable with good color match and contour. The EAC lumen was well maintained without stenosis or contracture, and the patient reported no further discomfort (Fig. 3C).
Discussion
Reconstruction of auricular and EAC defects following oncologic excision is challenging because of the region’s complex three-dimensional contour, thin skin, and limited local tissue availability [9]. In particular, defects involving the conchal bowl often expose cartilage and disrupt the natural curvature of the auricle, making both functional and aesthetic restoration essential.
The RDIF offers a distinct selective advantage in these cases, particularly for defects extending into the EAC. The retroauricular skin is thin and flexible, providing an ideal anatomical match for the EAC skin. Unlike skin grafts, which are prone to secondary contracture and often lead to canal stenosis, the RDIF provides stable, vascularized tissue that maintains canal patency without risk of significant shrinkage. Moreover, the reliable blood supply of the RDIF ensures stable flap survival even in cases where the underlying cartilage has been resected. The flap effectively fills the surgical defect, allowing for the successful restoration of the natural auricular contour.
In our two cases, the RDIF provided stable flap survival and preserved the natural auricular contour. EAC patency was also maintained, and no complications such as infection, necrosis, or stenosis occurred. The thin and flexible retroauricular skin blended well with the conchal surface, contributing to a favorable cosmetic result. The procedure could be performed under local anesthesia, which reduced perioperative burden and was beneficial for patients with underlying medical conditions. The surgical steps were straightforward, required no additional equipment, and were completed in a relatively short operation time. Adequate oncologic margins were obtained without difficulty, and perfusion of the flap remained stable. Postoperative discomfort was minimal, and healing progressed smoothly with a natural appearance.
From an oncologic standpoint, both cases achieved complete tumor clearance with histologically negative margins. The use of RDIF in this context allowed for both definitive closure and reliable surveillance of the operative field, since the flap maintains stable tissue characteristics over time.
In summary, the retroauricular RDIF represents a dependable, single-stage reconstructive option for moderate auricular and EAC defects following BCC excision. Its excellent vascularity, concealed donor site, and harmonious contour restoration make it a preferred technique when both aesthetic and functional outcomes are critical.
Notes
Acknowledgments
None
Author Contribution
Conceptualization: In Seok Moon. Data curation: Won Uk Lee. Formal analysis: Won Uk Lee. Investigation: In Seok Moon, Jeong Gum Lee. Methodology: In Seok Moon, Won Uk Lee. Project administration: Jeong Gum Lee. Resources: Jeong Gum Lee, Won Uk Lee. Software: Won Uk Lee. Supervision: In Seok Moon. Validation: In Seok Moon. Visualization: Won Uk Lee. Writing—original draft: Won Uk Lee. Writing—review & editing: all authors.
